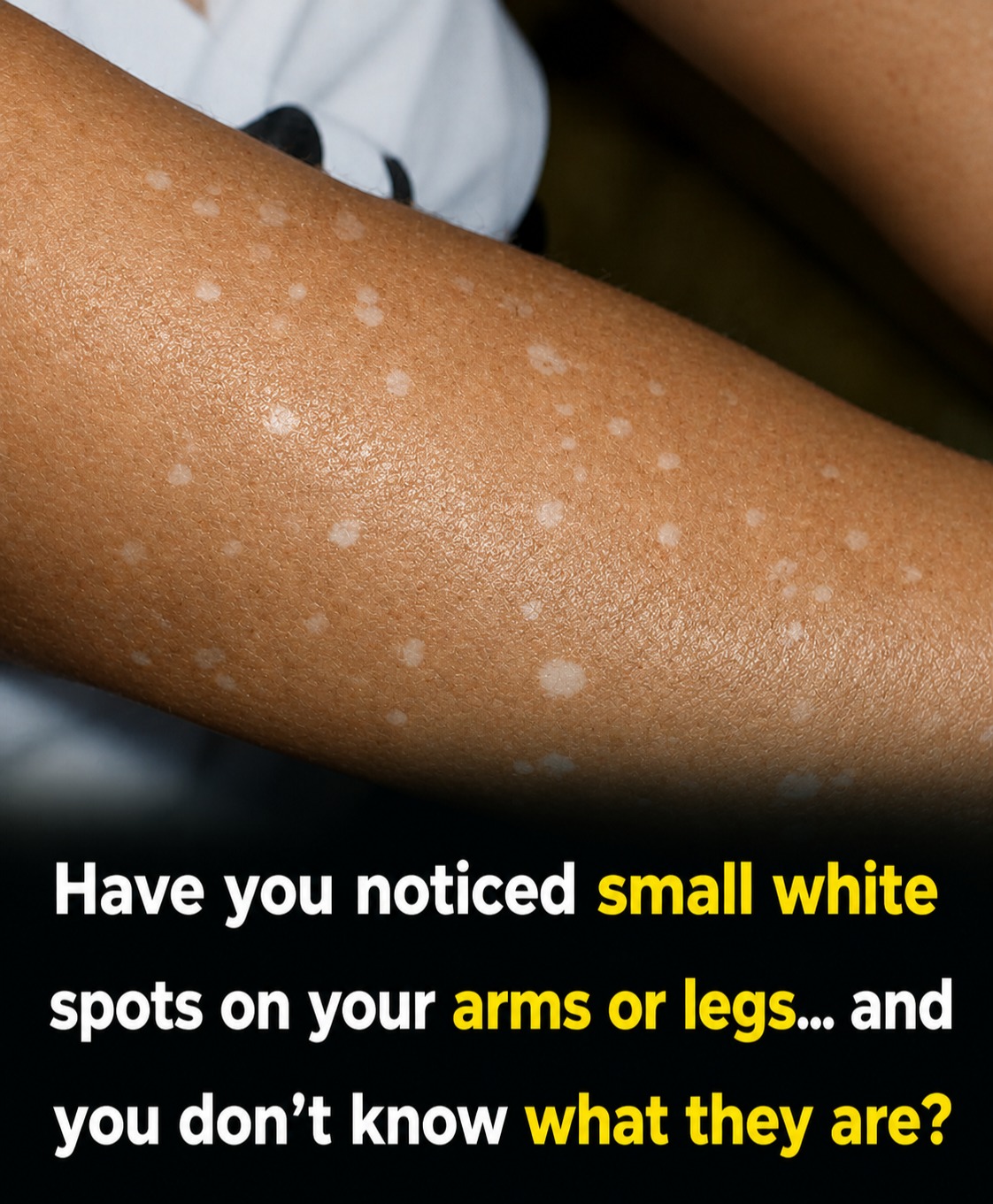
The human skin has amazing communication capabilities. It blushes if we feel embarrassed; it gives us goosebumps when we feel cold; and sometimes, it grows little mysterious white patches seemingly out of thin air.
Have you noticed little white spots or patches appearing on your skin lately? Don’t panic; you’re not alone! Most people’s first reaction to these patches is fear—they could be fungi, they could be permanent, and they could be an indication of some internal problem.
The good thing is that most small patches on the skin are actually harmless from a medical point of view. Nevertheless, taking into consideration that the skin plays such an important role in our confidence and appearance, figuring out the “why” behind all the changes is absolutely necessary. What happens is that there is some depletion of melanin, which gives the skin its natural color, or this substance stops being produced in certain areas.
We will go through all the causes behind the appearance of these spots, as well as find out how they develop and what can be done about them.
1. The Most Likely Culprit: Idiopathic Guttate Hypomelanosis (IGH)
If you are above the age of 30 and have seen very small, porcelain-like white spots on your shins or forearms, chances are that what you have is called Idiopathic Guttate Hypomelanosis (IGH). Though the name sounds scary, it is one of the most common skin problems.
In medical terms, “idiopathic” denotes the unknown cause of the problem, “guttate” is the term for the tear-drop shape, and “hypomelanosis” means the absence of pigment. As indicated by studies published in numerous dermatological periodicals, IGH is basically a manifestation of “aging of the skin” plus prolonged UV irradiation. The rays of the sun over decades may impair melanocytes (cells producing pigmentation) in isolated and localized sites; the cells just “shut down.”
Appearance: Pale patches in a flat and smooth form measuring from 2mm to 5mm across.
Location: Usually the shins, forearms, and occasionally the face or upper back.
According to the American Academy of Dermatology (AAD), IGH is not a precursor to skin cancer and is purely a cosmetic concern.
What can be done
As the cells responsible for producing the coloration in these areas often cease to function altogether, “repigmentation” is not an easy task. However, preventing additional exposure to the sun’s UV rays is essential to avoid developing more sunspots. Some dermatologists use topical retinoids or gentle dermabrasion to blend these sunspots together, but most individuals opt to leave them as they are.
2. The Living Landscape: Tinea Versicolor
But what about those cases where white spots aren’t caused by the sun, but by something else living on your skin? It’s a type of fungal infection called tinea versicolor that results from too much growth of yeast called Malassezia.
Malassezia resides on everybody’s skin; it is a normal part of our microbiota. Nevertheless, in hot and moist conditions, or when skin is especially oily, this yeast tends to overgrow. Once Malassezia overgrows, it starts producing an acid affecting the process of melanin formation. Thus, spots with reduced pigmentation (sometimes hyperpigmented spots) appear.
Appearance: White, pink, or light brown spots, having a thin and scaly coating. The latter can be easily spotted upon gentle scratching.
Behavior: Typically, such spots are more noticeable after being exposed to the sun as the yeast inhibits their tanning, whereas other skin remains darkened.
The Centers for Disease Control and Prevention (CDC) notes that this is one of the most frequent superficial fungal infections globally.
How to manage it
Tinea versicolor is easily treated with clotrimazole or miconazole cream from the local drug store. It is also suggested that individuals suffering from tinea versicolor use anti-dandruff shampoos which contain either selenium sulfide or ketoconazole, but they have to use them as a body wash instead. They have to apply this solution on the affected area, wait for five to ten minutes, and then wash it off.
Wikipedia
3. Pityriasis Alba: The Dry Skin Connection
Misdiagnosed as other, more severe illnesses, pityriasis alba is common in families with children and adolescents. In most cases, pityriasis alba is seen as a mild form of atopic dermatitis.
While in IGH there is smoothness, the patches in Pityriasis alba begin as red and scaly patches. After the inflammation goes down, there will be a pale and dry patch left behind. It is most prevalent among children suffering from asthma or hay fever.
Appearance: Circular or oval lesions found mostly on the cheeks, chin, or upper arms.
Seasonality: It becomes very apparent during the summertime. This is not due to exposure to the sun, but rather because the white spots do not tan, and thus, the contrast between the two becomes more pronounced.
DermNet NZ classifies this as a self-limiting condition, meaning it eventually goes away on its own as the child reaches adulthood.
Treatment and Care
The goal here is hydration. In this case, the treatment would involve the rehydration of the skin. It is recommended that you apply a thick moisturizing lotion without any smell two times a day. In case the patches appear red or irritated, then a hydrocortisone cream available over the counter could be applied for a couple of days.
4. Vitiligo: When the Immune System Intervenes
Perhaps the most well-known cause of white patches is Vitiligo. This is an autoimmune condition where the body’s immune system mistakenly attacks and destroys its own melanocytes.
Vitiligo is distinct because the loss of pigment is usually complete—the patches are “milky white” rather than just “pale.” It affects approximately 1% of the world’s population and can start at any age.
Appearance: Clearly outlined chalk-white patches that tend to be symmetrical, with matching locations such as the two elbows, both knees, or both sides of the face.
Course: It may be variable, where some individuals develop small patches that remain constant while others continue to spread for decades.
The NIAMS stresses that although vitiligo does not cause pain or is contagious, it has important psychological implications.
Modern Medical Breakthroughs
Vitiligo treatment has improved dramatically in the past few years. Not only does UVB light therapy and steroid creams provide relief, but there is also a brand-new group of medications called JAK inhibitors which help “shut down” the autoimmune response, thus enabling pigment to reappear. If you think that you might have vitiligo, visiting a dermatologist would be your best course of action.
Distinguishing the Difference: A Quick Reference
If you are trying to figure out which condition matches your skin, use this comparison table:
Feature IGH (Sun Spots) Tinea Versicolor Pityriasis Alba Vitiligo
Texture Smooth Slightly Scaly Dry/Rough Smooth
Edges Blurry/Small Defined Faded/Blurry Very Sharp
Itchiness Never Sometimes Rarely Never
Typical Age 30+ Teens/Young Adults Children Any
Sun Impact Caused by sun Made more visible Made more visible High burn risk
Essential Skin Care Strategies
Whether the cause is known or not, the treatment of any white spots must be approached with two strategies – keeping the skin protected and healthy.
The Non-Negotiable: SPF 30+
Once the skin loses its coloration, it loses one of its major forms of protection from DNA damage caused by sunburns. White patches burn quicker than normal skin does. Therefore, wear sunscreen every day without fail, even when the weather is gloomy, to prevent what dermatologists call a “contrast effect.”
Barrier Repair
In cases where you have Pityriasis Alba, or generally dry skin, the “moisture sandwich” method should work well for you. You can put on your hydration serum or just water on your skin first, then follow with a rich moisturizer that includes ceramides.
Balance Your Microbiome
In case you tend to get those fungal related skin spots (tinea versicolor), make sure you dress in cotton or linen clothes. Polyester or other synthetic fabrics hold sweat and heat close to your skin, causing a greenhouse effect for the yeast.
When to See a Professional
Even though the skin disorders mentioned above are among the most frequent, there are also less common skin disorders such as Lichen Sclerosus or even rare skin lymphoma that may be manifested by white spots on the body. If any of the following symptoms occur, it is advisable to consult a dermatologist:
Rapid and sudden appearance of the patches.
Patches cause thickening, pain, or bleeding of the skin.
Patches occur in the genital region.
Loss of color leads to severe emotional distress.
A dermatologist may use a Wood’s Lamp (a special UV light) to look at your skin in a dark room. Under this light, vitiligo glows a bright “blue-white,” while fungal infections may glow a dull yellow or green, allowing for an instant and accurate diagnosis.
*Medical Disclaimer: This article is for general informational and educational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Skin conditions can vary widely between individuals, and symptoms that look similar may have different underlying causes. Always seek the advice of a qualified healthcare provider or dermatologist with any questions you may have regarding a medical condition. Do not disregard professional medical advice or delay seeking it because of information you have read here.